4-minute read
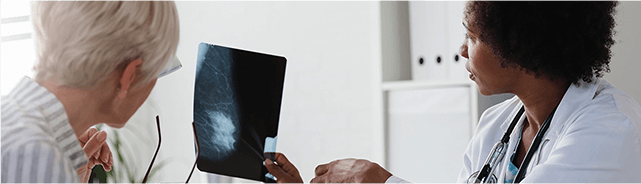
Oncologist reviewing x-ray of breast with patient
3 Facts Everyone Should Know About Metastatic Breast Cancer

For all the information about breast cancer available on the internet, surprisingly only a portion is dedicated to metastatic breast cancer (mBC). This information gap is troubling, as mBC is an aggressive and deadly stage of the disease. In this article, we’ll take a look at 3 key facts that everyone may not know about mBC—but should.
There are 4 main subtypes of breast cancer
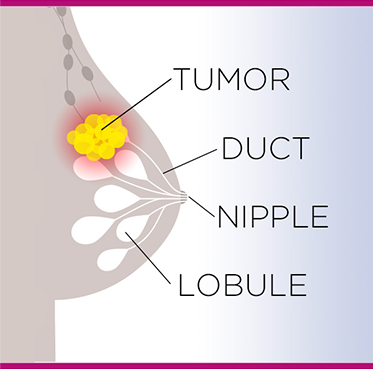
Anatomical diagram of breast cancer
Most people probably know that cancer occurs when cells of the body grow out of control. But what they may not know is that cancers are generally described by the location from which they originated. So, in the case of breast cancer, the tumor starts in breast tissue, such as the milk-producing glands, called lobules, or in the ducts that transport milk from the lobules to the nipple. If that cancer spreads to another body part, such as a lymph node or bone, it is called metastatic, and it is still considered breast cancer.1,2
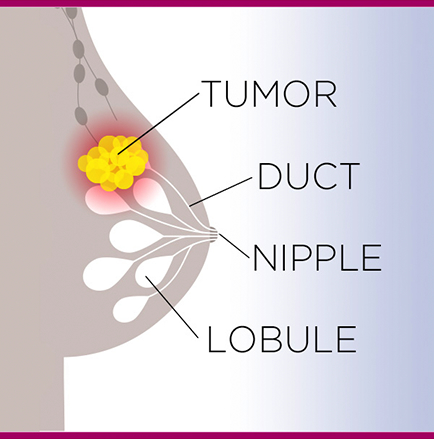
Anatomical diagram of breast cancer
What even fewer people may know is that there are 4 main subtypes of breast cancer.3 These are based on the presence or absence of receptors on the cancer’s cell surface and are involved in how the cancer grows.4-6 The severity of each type varies, but all of them have the potential to become metastatic.5,6
The cancerous cells that form in breast tissue may contain proteins that function as hormone receptors (HRs) for estrogen or progesterone, and if they do, those hormones can fuel cell growth.5 As its name suggests, human epidermal growth factor receptor 2 (HER2/neu) is another protein involved in normal cell growth, and it can be produced in larger-than-normal amounts in breast cancer.6
One of the first things a doctor does when investigating someone’s breast cancer is to determine whether or not these receptors are present in the cancerous cells. That receptor status provides insight into how the cancer can be expected to behave, and perhaps most importantly, how it may respond to treatment.5,6 Receptor status is a big deal.
Such a big deal, in fact, that the presence or absence of these receptors can describe more than 90% of the different types of breast cancer. Doctors break that down into 4 main groups*3,4:
- HR+/HER2/neu-, or “Luminal A” (~68%)
- HR-/HER2/neu-, or “Triple-negative breast cancer” (~10%)
- HR+/HER2/neu+, or “Luminal B” (~10%)
- HR-/HER2/neu+, or “HER2/neu-enriched” (~4%)
(The remaining ~7% comprises various forms that are very uncommon.)
*Percentage is for females. Based on data from cases in 2014-2018.4
Why is it so important to understand what type of breast cancer you have? Because of the complexities and nuances between subtypes, your doctor will develop a treatment plan specific to your receptor status.5,6

Let’s zoom out and look at mBC from a big-picture vantage point.
An estimated 155,000 people in the United States are living with mBC7
There are so many people in the country living with MBC that they could form a mid-sized city. Of the ~280,000 people diagnosed with breast cancer each year,8 about 6% will be metastatic at the time of diagnosis, and up to 30% of cases could eventually become metastatic.7
Notice that we’ve cited those numbers as people, and not women. While breast cancer affects primarily females, males can, in fact, get it. Men account for 1% of breast cancer cases and 1% of breast cancer deaths.9 The breast cancers that men get are often metastatic.10 mBC rates vary by race as well: African American women are more likely to be diagnosed than Americans of European ancestry and are 40% more likely to die from the disease.11 The racial disparity is particularly noticeable in younger women.11 Regardless of race, mBC is most often diagnosed between the ages of 45 and 65.12
Some researchers have estimated that ~80,000 people are diagnosed with metastatic breast cancer annually, though concrete numbers aren’t available.13 One number, however, is painfully certain: approximately 40,000 Americans die from mBC annually.8
If you or someone close to you was recently diagnosed with mBC, you’re not alone. Many others have gone through a similar experience, some of whom eagerly share guidance and support. You can find a curated list of great advocacy and support groups here: https://www.halaven.com/metastatic-breast-cancer/community-groups.
The survival rate for women diagnosed with mBC is improving14
There is reason for optimism: the survival rate is rising. Greater awareness and improvements in treatment have helped more women live longer following their mBC diagnosis.14 One can hope that the trend continues, and the women diagnosed today will live even longer.
It’s important to remember that these types of statistics provide an overview for the general population. An individual’s risk can vary for a wide range of factors, including age of diagnosis, ethnicity, cancer subtype, and more.14 These figures are helpful in understanding the disease in broad terms; they shouldn’t be misconstrued as a prediction of how long any individual may live after being diagnosed with mBC.
Adding it all up
mBC may be more common than you realize. It certainly warrants more awareness, given its severity. It’s also important to remember that on the other side of all the statistics the lives of real people are being affected every day. For every diagnosis, there is a family dealing with uncertainties and worries. One of the best ways to overcome those uncertainties is through education. If you’d like to learn more about mBC, please visit https://www.halaven.com/metastatic-breast-cancer/what-is-mbc.
 References:
References:
- Breast Cancer.org. What is breast cancer? Accessed May 3, 2021. https://www.breastcancer.org/symptoms/understand_bc/what_is_bc.
- National Cancer Institute. Metastatic cancer: when cancer spreads. Accessed May 3, 2021. https://www.cancer.gov/types/metastatic-cancer
- National Cancer Institute. Surveillance, Epidemiology, and End Results Program. Cancer Stat Facts: Female Breast Cancer Subtypes. Accessed May 17, 2021. https://seer.cancer.gov/statfacts/html/breast-subtypes.html
- Mayo Clinic. Breast cancer types: what your type means. Accessed May 3, 2021. https://www.mayoclinic.org/diseases-conditions/breast-cancer/in-depth/breast-cancer/art-20045654
- American Cancer Society. Breast cancer hormone receptor status. Accessed May 3, 2021. https://www.cancer.org/cancer/breast-cancer/understanding-a-breast-cancer-diagnosis/breast-cancer-hormone-receptor-status.html
- American Cancer Society. Breast cancer HER2 status. Accessed May 3, 2021. https://www.cancer.org/cancer/breast-cancer/understanding-a-breast-cancer-diagnosis/breast-cancer-her2-status.html
- Metastatic Breast Cancer Network. Most common statistics cited for MBC. Accessed May 3, 2021. http://mbcn.org/most-common-statistics-cited-for-mbc/
- National Cancer Institute. Surveillance, Epidemiology, and End Results Program. Cancer stat facts: female breast cancer. Accessed May 3, 2021. https://seer.cancer.gov/statfacts/html/breast.html
- American Cancer Society. Cancer Statistics Center. Breast. Accessed May 3, 2021. https://cancerstatisticscenter.cancer.org/?_ga=2.228442333.1968682772.1620144986-707333737.1620144986#!/cancer-site/Breast
- American Cancer Society. What is breast cancer in men? Accessed May 3, 2021. https://www.cancer.org/cancer/breast-cancer-in-men/about/what-is-breast-cancer-in-men.html
- Black Women's Health Imperative. What you need to know about breast cancer now. Accessed May 3, 2021. https://bwhi.org/2018/10/10/what-you-need-to-know-about-breast-cancer-nowpart-1-of-a-4-part-series-with-dr-lisa-newman/
- Metastatic Breast Cancer Network. Who gets breast cancer? Accessed May 3, 2021. http://mbcn.org/who-gets-breast-cancer/.
- METAvivor. Metastatic breast cancer statistics. Accessed May 3, 2021. https://www.metavivor.org/mbc-prep/metastatic-breast-cancer-statistics/
- American Cancer Society. Survival rates for breast cancer. Accessed May 3, 2021. https://www.cancer.org/cancer/breast-cancer/understanding-a-breast-cancer-diagnosis/breast-cancer-survival-rates.html